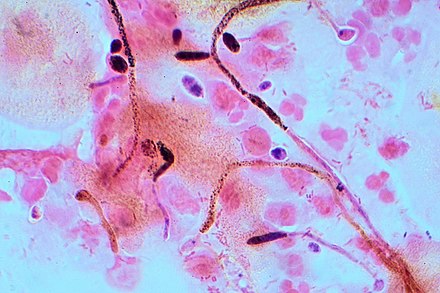
Dr. William Shaw's lab found that 60 to 70% of people with autism had overgrowth of Clostridia and Candida in their intestines, organisms that antibiotics leave behind while killing beneficial bacteria.
— The HighWire (@HighWireTalk) April 28, 2026
Treatment would clear the overgrowth and symptoms would improve, sometimes… pic.twitter.com/AJ6WVvaxDw
A recent clip from The HighWire (a health-focused show hosted by Del Bigtree) has been making the rounds on X. In it, biochemist Dr. William Shaw—former director of a lab that specialized in testing for metabolic and microbial imbalances—describes decades of work linking certain gut “bad guys” to autism and other brain-related conditions. The takeaway? In many cases, overgrowth of two common microbes (Clostridia bacteria and Candida yeast) seems to play a big role, and a measles vaccine may temporarily weaken the body’s ability to keep Candida in check. When the overgrowth is treated, symptoms can improve dramatically—sometimes even reverse—but they often return if the treatment stops. Here’s a clear, straightforward breakdown of what Shaw shared, why it matters, and what the science actually shows.
The Gut Problem in Autism (and Beyond)
Dr. Shaw’s lab analyzed urine and stool samples from thousands of children with autism. They found that 60 to 70 percent had unusually high levels of Clostridia bacteria and Candida yeast in their intestines. These aren’t rare invaders—they live in all of us—but when “good” bacteria get wiped out (often by antibiotics), the bad ones can explode in numbers.
- Clostridia produce a chemical called HPHPA that can cross into the brain and mess with dopamine, a key chemical for mood, focus, and behavior.
- Candida (the same yeast behind thrush or stubborn infections) thrives in the same disrupted gut environment.
The pattern isn’t limited to autism. Shaw’s team saw the same Clostridia/Candida overgrowth signature in many other psychiatric conditions.
What Happens When You Treat It?
Here’s where it gets striking: When doctors targeted these microbes with the right antifungal or antibiotic (guided by lab tests), symptoms often improved fast—sometimes within weeks. Kids with autism showed better eye contact, language, and behavior. In one documented case of severe schizophrenia, a targeted antibiotic led to a complete reversal of psychosis.
But there was a catch. Once the treatment ended, the overgrowth—and the symptoms—came roaring back in many cases. Why couldn’t the body keep the microbes under control on its own?
The Vaccine Piece of the Puzzle
Shaw points to a 2001 study from researchers involving Bangladeshi infants (published in the journal Vaccine). They gave measles vaccine to infants and checked immune responses six weeks later. The surprising result: the children’s cell-mediated immunity (a key defense measured by skin tests) against Candida dropped significantly—but only against Candida. Responses to every other germ they tested stayed normal.
In plain English: the vaccine appeared to create a temporary “blind spot” in the immune system specifically for this one yeast. If Candida was already trying to overgrow (thanks to antibiotics or other factors), the body lost its best tool for fighting it off. The effect was temporary in the study, but Shaw’s clinical experience suggested it could leave some children more vulnerable long-term.
(Note: This was a small study on immune markers, not a direct proof that vaccines cause autism. It simply showed a specific, measurable change in one immune pathway.)
Real-World Examples and a Famous Case Study
The interview highlights a 2020 case report co-authored by Shaw and Dr. Sidney Baker. A child with autism symptoms and lab evidence of fungal (Aspergillus) overgrowth in the gut received a strong antifungal drug. Within months, his autism symptoms vanished completely, and he went on to excel in school, sports, and music. The fungal markers dropped in tandem with the behavioral improvement.
Parents in the replies to the X post echoed similar stories: kids who improved dramatically on antifungals or gut-healing protocols, only to regress when treatment stopped or after more antibiotics. Some also noted improvements in schizophrenia, ADHD-like symptoms, or even adult issues after addressing gut yeast and bacteria.
Why This Matters—and Why It’s Controversial
Mainstream medicine now widely accepts that gut microbiome imbalances are common in autism (up to 70-90% of autistic kids have GI problems). Researchers are actively studying microbiome therapies like fecal transplants, targeted probiotics, and diet changes. Clostridia metabolites like HPHPA have been replicated in multiple studies as a biomarker in autism and some psychiatric disorders.
What’s still debated:
- Is the gut issue a cause of autism, or just a common side effect?
- How big a role do vaccines, antibiotics, or environmental factors play?
- Can these treatments produce lasting cures, or only symptom relief while the therapy continues?
Dr. Shaw’s work sits at the edge of conventional and integrative medicine. Some of his earlier vaccine-related claims have drawn criticism, but the specific studies he cites here are published and verifiable. The broader idea—that gut microbes influence the brain via the “gut-brain axis”—is now a hot field in neuroscience.
Bottom Line
This clip isn’t claiming a single “cure” for autism or mental illness. It’s presenting a practical, testable hypothesis: in a large subset of cases, a treatable gut imbalance (Clostridia + Candida) driven partly by immune changes may be fueling symptoms. When cleared, some people improve dramatically. The research raises hopeful questions about simple lab tests, targeted antimicrobials, probiotics, and diet as tools that could help many families—especially when standard approaches fall short.
If you or someone you know is dealing with autism, schizophrenia, or related gut/brain issues, the takeaway from Shaw’s decades of lab work is simple: ask your doctor about organic acids testing (which flags these microbial markers) and consider a microbiome-focused evaluation. Science is still catching up, but real people in the comments and case reports say the results have been life-changing.
Fascinating stuff—and a reminder that sometimes the answers hide in the most overlooked place: our own intestines.
Perhaps a speical diet could help?