The Centers for Disease Control (CDC) just released this report on so-called “superbugs” or threats that are resistant to antibiotics. Read this report to find out just how many of these superbugs are out there and how many Americans are dying from them every year.
2019 AR Threats Report
CDC’s Antibiotic Resistance Threats in the United States, 2019 (2019 AR Threats Report) includes the latest national death and infection estimates that underscore the continued threat of antibiotic resistance in the U.S.
According to the report, more than 2.8 million antibiotic-resistant infections occur in the U.S. each year, and more than 35,000 people die as a result. In addition, 223,900 cases of Clostridioides difficile occurred in 2017 and at least 12,800 people died.
Dedicated prevention and infection control efforts in the U.S. are working to reduce the number of infections and deaths caused by antibiotic-resistant germs, but the number of people facing antibiotic resistance is still too high. More action is needed to fully protect people.
CDC is concerned about rising resistant infections in the community, which can put more people at risk, make spread more difficult to identify and contain, and threaten the progress made to protect patients in healthcare. The emergence and spread of new forms of resistance remains a concern.
The report lists 18 antibiotic-resistant bacteria and fungi into three categories based on level of concern to human health—urgent, serious, and concerning—and highlights:
- Estimated infections and deaths since the 2013 report
- Aggressive actions taken
- Gaps slowing progress
The report also includes a Watch List with three threats that have not spread resistance widely in the U.S. but could become common without a continued aggressive approach.
The 2019 AR Threats Report is intended to:
- Serve as a reference for information on antibiotic resistance
- Provide the latest U.S. antibiotic resistance burden estimates for human health
- Highlight emerging areas of concern and additional action needed
In 2013, CDC published the first AR Threats Report, which sounded the alarm to the danger of antibiotic resistance. The report stated that each year in the U.S. at least 2 million people get an antibiotic-resistant infection, and at least 23,000 people die. The 2013 AR Threats Report helped inform the National Action Plan for Combating Antibiotic-Resistant Bacteria. The 2013 and 2019 reports do not include viruses (e.g., HIV, influenza) or parasites.
Bacteria and Fungi Listed in the 2019 AR Threats Report
Urgent Threats
- Carbapenem-resistant Acinetobacter
- Candida auris
- Clostridioides difficile
- Carbapenem-resistant Enterobacteriaceae
- Drug-resistant Neisseria gonorrhoeae
Serious Threats
- Drug-resistant Campylobacter
- Drug-resistant Candida
- ESBL-producing Enterobacteriaceae
- Vancomycin-resistant Enterococci (VRE)
- Multidrug-resistant Pseudomonas aeruginosa
- Drug-resistant nontyphoidal Salmonella
- Drug-resistant Salmonella Serotype Typhi
- Drug-resistant Shigella
- Methicillin-resistant Staphylococcus aureus (MRSA)
- Drug-resistant Streptococcus pneumoniae
- Drug-resistant Tuberculosis
Concerning Threats
Watch List
- Azole-resistant Aspergillus fumigatus
- Drug-resistant Mycoplasma genitalium
- Drug-resistant Bordetella pertussis
Urgent Threats
Carbapenem-resistant Acinetobacter
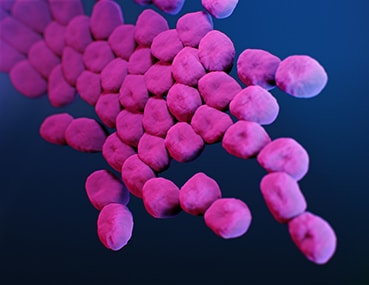
Type: Bacteria
About: Carbapenem-resistant Acinetobacter cause pneumonia and wound, bloodstream, and urinary tract infections. Nearly all these infections happen in patients who recently received care in a healthcare facility.
Estimated cases in hospitalized patients in 2017: 8,500
Estimated deaths in 2017: 700
Learn more: CDC’s Acinetobacter website
Download data: Carbapenem-resistant Acinetobacter Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Candida auris (C. auris)

Type: Fungus
About: C. auris is an emerging multidrug-resistant yeast. It can cause severe infections and spreads easily between hospitalized patients and nursing home residents.
Clinical cases in 2018: 323
Learn more: CDC’s C. auris website
Download data: Drug-resistant C. auris Pathogen Page pdf icon[PDF – 2 pages]
Clostridioides difficile (C. difficile)
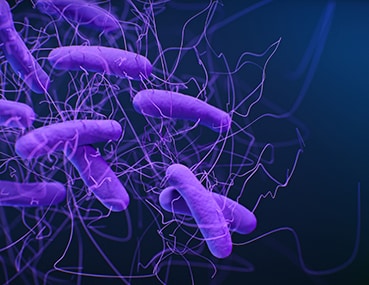
Type: Bacteria
Also known as: C. difficile or C. diff, previously Clostridium difficile
About: C. difficile causes life-threatening diarrhea and colitis (an inflammation of the colon), mostly in people who have had both recent medical care and antibiotics.
Infections per year: 223,900
Deaths per year: 12,800
Learn more: CDC’s C. difficile website
Download data: C. difficile Pathogen Page pdf icon[PDF – 2 pages]
Carbapenem-resistant Enterobacteriaceae (CRE)
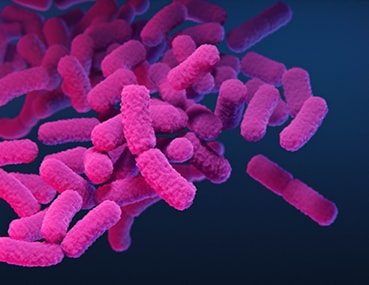
Type: Bacteria
Also known as: Nightmare bacteria
About: CRE are a major concern for patients in healthcare facilities. Some Enterobacteriaceae (a family of germs) are resistant to nearly all antibiotics, leaving more toxic or less effective treatment options.
Estimated cases in hospitalized patients in 2017: 13,100
Estimated deaths in 2017: 1,100
Learn more: CDC’s CRE website
Download data: CRE Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Neisseria gonorrhoeae (N. gonorrhoeae)
Type: Bacteria
Also known as: Drug-resistant gonorrhea
About: N. gonorrhoeae causes the sexually transmitted disease gonorrhea that can result in life-threatening ectopic pregnancy and infertility, and can increase the risk of getting and giving HIV.
Estimated drug-resistant infections per year: 550,000
Learn more: CDC’s antibiotic-resistant gonorrhea website
Download data: Drug-resistant N. gonorrhoeae Pathogen Page pdf icon[PDF – 2 pages]Top of Page
Serious Threats
Drug-resistant Campylobacter
Type: Bacteria
Also known as: Campy
About: Campylobacter usually causes diarrhea (often bloody), fever, and abdominal cramps, and can spread from animals to people through contaminated food, especially raw or undercooked chicken.
Drug-resistance infections per year: 448,400
Estimated deaths per year: 70
Learn more: CDC’s Campylobacter website
Download data: Drug-resistant Campylobacter Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Candida Species
Type: Fungus
About: Dozens of Candida species—a group of fungi—cause infections, ranging from mild oral and vaginal yeast infections to severe invasive infections. Many are resistant to the antifungals used to treat them.
Estimated cases in hospitalized patents in 2017: 34,800
Deaths in 2017: 1,700
Learn more: CDC’s Candida website
Download data: Drug-resistant Candida Species Pathogen Page pdf icon[PDF – 2 pages]
Extended-spectrum Beta-lactamase (ESBL) producing Enterobacteriaceae
Type: Bacteria
Also known as: Extended-spectrum β-lactamase
About: ESBL-producing Enterobacteriaceae are a concern in healthcare settings and the community. They can spread rapidly and cause or complicate infections in healthy people.
- ESBLs are enzymes that break down commonly used antibiotics, such as penicillins and cephalosporins, making them ineffective.
Estimated cases in hospitalized patients in 2017: 197,400
Estimated deaths in 2017: 9,100
Learn more: CDC’s ESBL-producing Enterobacteriaceae website
Download data: ESBL-producing Enterobacteriaceae Pathogen Page pdf icon[PDF – 2 pages]
Vancomycin-resistant Enterococcus (VRE)
Type: Bacteria
About: Enterococci can cause serious infections for patients in healthcare settings, including bloodstream, surgical site, and urinary tract infections.
Estimated cases in hospitalized patients in 2017: 54,500
Estimated deaths in 2017: 5,400
Learn more: CDC’s VRE in Healthcare Settings website
Download data: VRE Pathogen Page pdf icon[PDF – 2 pages]
Multidrug-resistant Pseudomonas aeruginosa (P. aeruginosa)
Type: Bacteria
About: P. aeruginosa infections usually occur in people with weakened immune systems, and can be particularly dangerous for patients with chronic lung diseases.
Estimated cases in hospitalized patients in 2017: 32,600
Estimated deaths in 2017: 2,700
Learn more: CDC’s P. aeruginosa website
Download data: Multidrug-resistant P. aeruginosa Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant nontyphoidal Salmonella
Type: Bacteria
About: Nontyphoidal Salmonella can spread from animals to people through food, and usually causes diarrhea, fever, and abdominal cramps. Some infections spread to the blood and can have life-threatening complications.
Estimated drug-resistant infections per year: 212,500
Estimated deaths per year: 70
Learn more: CDC’s Salmonella website
Download data: Drug-resistant nontyphoidal Salmonella Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Salmonella Serotype Typhi
Type: Bacteria
Also known as: Typhoid fever
About: Salmonella Typhi causes a serious disease called typhoid fever, which can be life-threatening. Most people in the U.S. become infected while traveling to countries where the disease is common.
Estimated drug-resistant infections per year: 4,100
Estimated deaths per year: Less than 5
Learn more: CDC’s Typhoid Fever website
Download data: Drug-resistant Salmonella Serotype Typhi Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Shigella
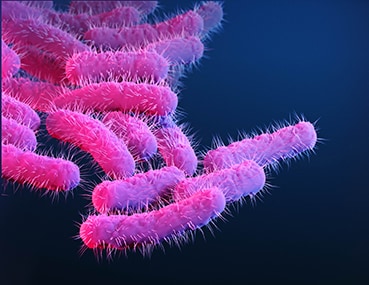
Type: Bacteria
About: Shigella spreads in feces through direct contact or through contaminated surfaces, food, or water, and most people infected with Shigella develop diarrhea, fever, and stomach cramps.
Estimated drug-resistant infections per year: 77,000
Estimated deaths per year: Less than 5
Learn more: CDC’s Shigella website
Download data: Drug-resistant Shigella Pathogen Page pdf icon[PDF – 2 pages]
Methicillin-resistant Staphylococcus aureus (S. aureus) (MRSA)
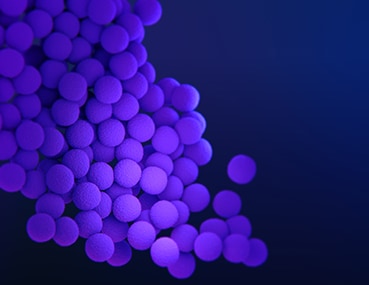
Type: Bacteria
Also known as: Resistant staph (short for Staphylococcus)
About: S. aureus are common bacteria that spread in healthcare facilities and the community. MRSA can cause difficult-to-treat staph infections because of resistance to some antibiotics.
Estimated cases in hospitalized patients in 2017: 323,700
Estimated deaths in 2017: 10,600
Learn more: CDC’s MRSA website
Download data: MRSA Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Streptococcus pneumoniae (S. pneumonia)
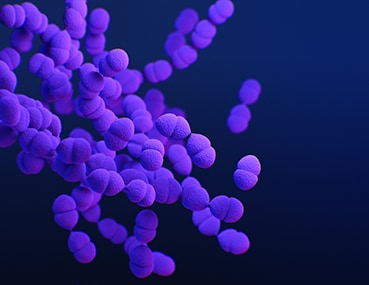
Type: Bacteria
Also known as: Pneumococcus
About: S. pneumoniae causes pneumococcal disease, which can range from ear and sinus infections to pneumonia and bloodstream infections.
Estimated infections in 2014: 900,00
Estimated deaths in 2014: 3,600
Learn more: CDC’s S. pneumoniae website
Download data: Drug-resistant S. pneumoniae Pathogen Page pdf icon[PDF – 2 pages]
Drug-resistant Tuberculosis
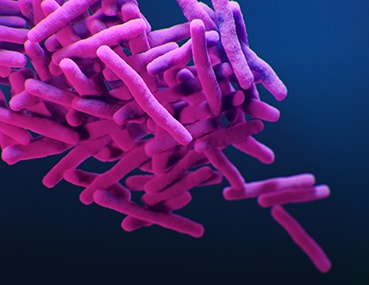
Type: Bacteria
Also known as: TB, multidrug-resistant TB (MDR TB), or extensively drug-resistant TB (XDR TB), Mycobacterium tuberculosis (M. tuberculosis)
About: TB is caused by the bacteria M. tuberculosis, and is among the most common infectious diseases and a frequent cause of death worldwide.
Drug-resistant TB cases in 2011: 847
Deaths in 2017: 62
Learn more: CDC’s TB website
Download data: Drug-resistant TB Pathogen Page pdf icon[PDF – 2 pages]Top of Page
Concerning Threats
Erythromycin-resistant Group A Streptococcus
Type: Bacteria
Also known as: Resistant group A strep, GAS
About: GAS can cause many different infections that range from minor illnesses to serious and deadly diseases, including strep throat, pneumonia, flesh-eating infections, and sepsis.
Estimated drug-resistant infections in 2017: 5,400
Estimated deaths in 2017: 450
Learn more: CDC’s GAS website
Download data: GAS Pathogen Page pdf icon[PDF – 2 pages]
Clindamycin-resistant Group B Streptococcus
Type: Bacteria
Also known as: Resistant group B strep, GBS
About: GBS can cause severe illness in people of all ages.
Estimated drug-resistant infections in 2016: 13,000
Estimated deaths in 2016: 720
Learn more: CDC’s GBS website
Download data: GBS Pathogen Page pdf icon[PDF – 2 pages]Top of Page
Watch List
Azole-resistant Aspergillus fumigatus
Aspergillus is a fungus that can cause life-threatening infections in people with weakened immune systems. These infections are treated with antifungals called azoles. Azoles are also increasingly used in agriculture to prevent and treat fungal diseases in crops. Azole use in human medicine and agriculture can contribute to resistance to antifungal medicines.
Drug-resistant Mycoplasma genitalium (M. genitalium)
M. genitalium bacteria are sexually transmitted and can cause urethritis in men (inflammation of the urethra) and may cause cervicitis in women (inflammation of the cervix). Few antibiotics are available to treat M. genitalium infections. Resistance to azithromycin, which has been recommended for treatment, is high across the globe.
Drug-resistant Bordetella pertussis (B. pertussis)
Pertussis, a respiratory illness commonly known as whooping cough, is a very contagious disease caused by a type of bacteria called B. pertussis. It can cause serious and sometimes deadly complications, especially in babies.