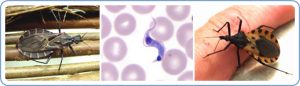
Chagas disease is named after the Brazilian physician Carlos Chagas, who discovered the disease in 1909. It is caused by the parasite Trypanosoma cruzi, which is transmitted to animals and people by insect vectors and is found only in the Americas. Chagas disease (T. cruzi infection) is also referred to as American trypanosomiasis. (CDC info here.) It is a leading cause of heart failure in Latin America – and it’s headed North.
In the United States, Chagas disease is considered one of the neglected parasitic infections (NPI), a group of five parasitic diseases that have been targeted by CDC for public health action. Right now, Texas is particularly afflicted with these bugs which are attacking children and dogs, often to deadly effect.
Infection is most commonly acquired through contact with the feces of an infected triatomine bug (or “kissing bug”), a blood-sucking insect that feeds on humans and animals. Assassin bugs (or kissing bugs) get their names from their habit of biting humans on the face near the lips.
Infection can also occur from:
- mother-to-baby (congenital),
- contaminated blood products (transfusions),
- an organ transplanted from an infected donor,
- laboratory accident, or
- contaminated food or drink (rare)
Chagas disease is endemic throughout much of Mexico, Central America, and South America where an estimated 8 million people are infected. In these countries, spraying is conducted. The triatomine bug thrives under poor housing conditions (for example, mud walls, thatched roofs), so in endemic countries, people living in rural areas are at greatest risk for acquiring infection. Public health efforts aimed at preventing transmission have decreased the number of newly infected people and completely halted vectorborne transmission in some areas. Infection acquired from blood products, organ transplantation, or congenital transmission continues to pose a threat.
Assassin bugs like hanging out near their prey— mammals (including humans) with vertebrae — from which they can suck blood. During late spring and summer, they leave their usual nests in the woods (near rodents) and go in search of mates and new refuges. Along the way, kissing bugs are attracted to bright lights on houses at night. They work their way into homes and search out dark, cool places to stay during the day, only leaving again at night for food. They particularly like hiding between mattresses. (Apartment Therapy)
By applying published seroprevalence figures to immigrant populations, CDC estimates that more than 300,000 persons with Trypanosoma cruzi infection live in the United States. Most people with Chagas disease in the United States acquired their infections in endemic countries. Although there are triatomine bugs in the U.S. , only rare vectorborne cases of Chagas disease have been documented.
Chagas disease has an acute and a chronic phase. If untreated, infection is lifelong.
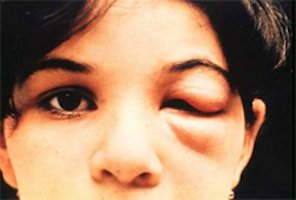
Acute Chagas disease occurs immediately after infection, may last up to a few weeks or months, and parasites may be found in the circulating blood. Infection may be mild or asymptomatic. There may be fever or swelling around the site of inoculation (where the parasite entered into the skin or mucous membrane). Rarely, acute infection may result in severe inflammation of the heart muscle or the brain and lining around the brain.
Following the acute phase, most infected people enter into a prolonged asymptomatic form of disease (called “chronic indeterminate”) during which few or no parasites are found in the blood. During this time, most people are unaware of their infection. Many people may remain asymptomatic for life and never develop Chagas-related symptoms. However, an estimated 20 – 30% of infected people will develop debilitating and sometimes life-threatening medical problems over the course of their lives.
Complications of chronic Chagas disease may include:
- heart rhythm abnormalities that can cause sudden death;
- a dilated heart that doesn’t pump blood well;
- a dilated esophagus or colon, leading to difficulties with eating or passing stool.
In people who have suppressed immune systems (for example, due to AIDS or chemotherapy), Chagas disease can reactivate with parasites found in the circulating blood. This occurrence can potentially cause severe disease.
The diagnosis of Chagas disease can be made by observation of the parasite in a blood smear by microscopic examination. A thick and thin blood smear are made and stained for visualization of parasites. However, a blood smear works well only in the acute phase of infection when parasites are seen circulating in blood.
Treatment for Chagas disease is recommended for all people diagnosed with an acute infection, congenital infection, and for those with suppressed immune systems, and for all children with chronic infection. Adults with chronic infection may also benefit from treatment.
For cardiac or gastrointestinal problems resulting from Chagas disease, symptomatic treatment may be helpful. Patients should consult with their primary health care provider. Some patients may be referred to a specialist, such as a cardiologist, gastroenterologist, or infectious disease specialist.
In the U.S., medication for Chagas is available only through CDC. Your health care provider can talk with CDC staff about whether and how you should be treated.
Avoidance:
- Seal any cracks or crevices to keep them from entering the home.
- Clear the perimeter around your home of leaves and burn any rodent nests.
- Make sure you don’t have any gaps underneath your exterior doors.
- Swap out regular lightbulbs for yellow bug safe ones instead.
- Keep screens on all your windows and doors.
- If you find assassin bugs in the home, or around the house, consider calling pest control to spray insecticide and notify local health authorities.